Other Addictions
Other Addictions
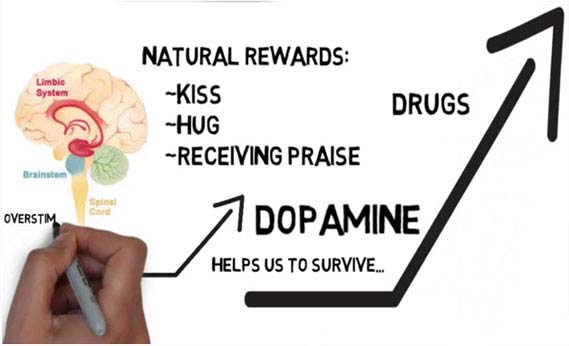
Addiction is a brain disorder characterized by compulsive engagement in rewarding stimuli, despite adverse consequences. Despite the involvement of a number of psychosocial factors, a biological process – one which is induced by repeated exposure to an addictive stimulus – is the core pathology that drives the development and maintenance of an addiction.
The two properties that characterize all addictive stimuli are that they are reinforcing (i.e., they increase the likelihood that a person will seek repeated exposure to them) and intrinsically rewarding (i.e., they are perceived as being inherently positive, desirable, and pleasurable).
Addiction is a disorder of the brain's reward system which arises through transcriptional and epigenetic mechanisms and occurs over time from chronically high levels of exposure to an addictive stimulus (e.g., morphine, cocaine, sexual intercourse, gambling, etc.). ΔFosB, a gene transcription factor, is a critical component and common factor in the development of virtually all forms of behavioral and drug addictions. Two decades of research into ΔFosB's role in addiction have demonstrated that addiction arises, and the associated compulsive behavior intensifies or attenuates, along with the genetic overexpression of ΔFosB in the D1-type medium spiny neurons of the nucleus accumbens. Due to the causal relationship between ΔFosB expression and addictions, it is used preclinically as an addiction biomarker. ΔFosB expression in these neurons directly and positively regulates drug self-administration and reward sensitization through positive reinforcement, while decreasing sensitivity to aversion.
Addiction exacts a high toll on individuals and society as a whole through the direct adverse effects of drugs, associated healthcare costs, long-term complications (e.g., lung cancer with smoking tobacco, liver cirrhosis with drinking alcohol, or meth mouth from intravenous methamphetamine), the functional consequences of altered neural plasticity in the brain, and the consequent loss of productivity.141516 Classic hallmarks of addiction include impaired control over substances or behavior, preoccupation with substance or behavior, and continued use despite consequences.17Habits and patterns associated with addiction are typically characterized by immediate gratification (short-term reward), coupled with delayed deleterious effects (long-term costs).
Examples of drug and behavioral addictions include: alcoholism, amphetamine addiction, cocaine addiction, nicotine addiction, opiate addiction, food addiction, gambling addiction, and sexual addiction. The only behavioral addiction recognized by the DSM-5 is gambling addiction. The term addiction is misused frequently to refer to other compulsive behaviors or disorders, particularly dependence, in news media. An important distinction between drug addiction and dependence is that drug dependence is a disorder in which cessation of drug use results in an unpleasant state of withdrawal, which can lead to further drug use. Addiction is the compulsive use of a substance or performance of a behavior that is independent of withdrawal.
Psychological therapy

Psychoanalysis, a psychotherapeutic approach to behavior change developed by Sigmund Freud and modified by his followers, has also offered an explanation of substance abuse. This orientation suggests the main cause of the addiction syndrome is the unconscious need to entertain and to enact various kinds of homosexual and perverse fantasies and at the same time to avoid taking responsibility for this. It is hypothesized specific drugs facilitate specific fantasies and using drugs is considered to be a displacement from, and a concomitant of, the compulsion to masturbate while entertaining homosexual and perverse fantasies. The addiction syndrome is also hypothesized to be associated with life trajectories that have occurred within the context of traumatogenic processes, the phases of which include social, cultural and political factors, encapsulation, traumatophilia, and masturbation as a form of self-soothing.
Relapse prevention

An influential cognitive-behavioral approach to addiction recovery and therapy has been Alan Marlatt’s (1985) Relapse Prevention approach. Marlatt describes four psychosocial processes relevant to the addiction and relapse processes: self-efficacy, outcome expectancies, attributions of causality, and decision-making processes. Self-efficacy refers to one’s ability to deal competently and effectively with high-risk, relapse-provoking situations. Outcome expectancies refer to an individual’s expectations about the psychoactive effects of an addictive substance. Attributions of causality refer to an individual’s pattern of beliefs that relapse to drug use is a result of internal, or rather external, transient causes (e.g., allowing oneself to make exceptions when faced with what are judged to be unusual circumstances). Finally, decision-making processes are implicated in the relapse process as well.
Substance use is the result of multiple decisions whose collective effects result in consumption of the intoxicant. Furthermore, Marlatt stresses some decisions—referred to as apparently irrelevant decisions—may seem inconsequential to relapse, but may actually have downstream implications that place the user in a high-risk situation.
For example: As a result of heavy traffic, a recovering alcoholic may decide one afternoon to exit the highway and travel on side roads. This will result in the creation of a high-risk situation when he realizes he is inadvertently driving by his old favorite bar. If this individual is able to employ successful coping strategies, such as distracting himself from his cravings by turning on his favorite music, then he will avoid the relapse risk (PATH 1) and heighten his efficacy for future abstinence. If, however, he lacks coping mechanisms—for instance, he may begin ruminating on his cravings (PATH 2)—then his efficacy for abstinence will decrease, his expectations of positive outcomes will increase, and he may experience a lapse—an isolated return to substance intoxication. So doing results in what Marlatt refers to as the Abstinence Violation Effect, characterized by guilt for having gotten intoxicated and low efficacy for future abstinence in similar tempting situations. This is a dangerous pathway, Marlatt proposes, to full-blown relapse.
Cognitive therapy

An additional cognitively-based model of substance abuse recovery has been offered by Aaron Beck, the father of cognitive therapy and championed in his 1993 book, Cognitive Therapy of Substance Abuse.29 This therapy rests upon the assumption addicted individuals possess core beliefs, often not accessible to immediate consciousness (unless the patient is also depressed). These core beliefs, such as “I am undesirable,” activate a system of addictive beliefs that result in imagined anticipatory benefits of substance use and, consequentially, craving. Once craving has been activated, permissive beliefs (“I can handle getting high just this one more time”) are facilitated. Once a permissive set of beliefs have been activated, then the individual will activate drug-seeking and drug-ingesting behaviors. The cognitive therapist’s job is to uncover this underlying system of beliefs, analyze it with the patient, and thereby demonstrate it’s dysfunctional. As with any cognitive-behavioral therapy, homework assignments and behavioral exercises serve to solidify what is learned and discussed during treatment.
Emotion regulation and mindfulness

A growing literature is demonstrating the importance of emotion regulation in the treatment of substance abuse. Considering that nicotine and other psychoactive substances such as cocaine activate similar psychopharmacological pathways, an emotion regulation approach may be applicable to a wide array of substance abuse. Proposed models of affect-driven tobacco use have focused on negative reinforcement as the primary driving force for addiction; according to such theories, tobacco is used because it helps one escape from the undesirable effects of nicotine withdrawal or other negative moods. Acceptance and commitment therapy (ACT), is showing evidence that it is effective in treating substance abuse, including the treatment of poly-substance abuse and cigarette smoking. Mindfulness programs that encourage patients to be aware of their own experiences in the present moment and of emotions that arise from thoughts, appear to prevent impulsive/compulsive responses. Research also indicates that mindfulness programs can reduce the consumption of substances such as alcohol, cocaine, amphetamines, marijuana, cigarettes and opiates.
Behavioral models
Behavioral models make use of principles of functional analysis of drinking behavior. Behavior models exists for both working with the substance abuser (Community Reinforcement Approach) and their family (Community Reinforcement Approach and Family Training). Both these models have had considerable research success for both efficacy and effectiveness. This model lays much emphasis on the use of problem solving techniques as a means of helping the addict to overcome his addiction.